Neural Energy Landscapes Predict Working Memory Decline After Brain Tumor Resection
Abstract: Surgical resection is the primary treatment option for brain tumor patients, but it carries the risk of postoperative cognitive dysfunction. This study investigates how tumor-induced alterations in presurgical neural dynamics relate to postoperative working memory decline. We analyzed functional magnetic resonance imaging (fMRI) of brain tumor patients before surgery and extracted energy landscapes of high-order brain interactions. We then examined the relation between these energy features and postoperative working memory performance using statistical and machine learning (random forest) models. Patients with lower postoperative working memory scores exhibited fewer but more extreme transitions between local energy minima and maxima, whereas patients with higher scores showed more frequent but less extreme shifts. Furthermore, the presurgical high-order energy features were able to accurately predict postoperative working memory decline with a mean accuracy of 90\%, F1 score of 87.5\%, and an AUC of 0.95. Our study suggests that the brain tumor-induced disruptions in high-order neural dynamics before surgery are predictive of postoperative working memory decline. Our findings pave the path for personalized surgical planning and targeted interventions to mitigate cognitive risks associated with brain tumor resection.
Paper Prompts
Sign up for free to create and run prompts on this paper using GPT-5.
Top Community Prompts
Explain it Like I'm 14
What this paper is about
This paper asks a simple but important question: can we look at how a person’s brain works before a brain tumor surgery and predict who might have trouble with working memory afterward? Working memory is like your brain’s “sticky note”—it helps you keep track of information for a short time, like remembering a phone number long enough to type it in.
The researchers use a special way of looking at brain activity called an “energy landscape,” which turns complex brain signals into a kind of map with valleys and hills. Valleys are stable brain states, and hills are less stable ones. By studying how the brain moves across this map, they try to predict memory problems after surgery.
The main goals and questions
- Can patterns in brain activity before surgery predict who will have lower working memory after surgery?
- Are “high‑order” patterns (how groups of brain regions work together) better at predicting outcomes than simple pair‑to‑pair connections?
- Do certain movement patterns across the energy landscape—like how often and how strongly the brain jumps between states—relate to later memory performance?
How the study was done (in everyday language)
They used resting‑state fMRI, which is like taking a movie of the brain’s activity while a person lies still with eyes closed. The idea is to see how different parts of the brain naturally “chat” with each other.
Here’s their approach, step by step:
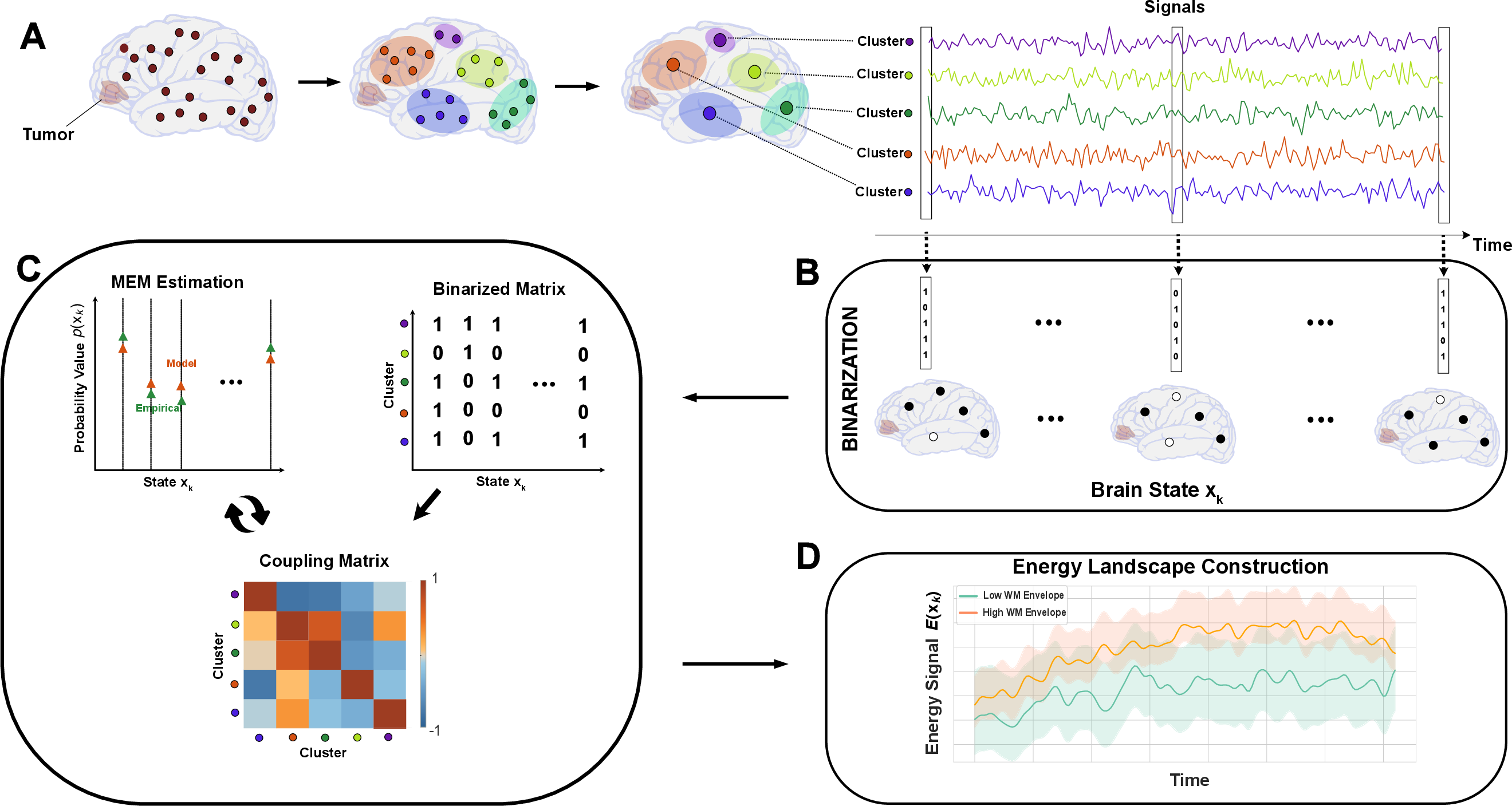
- Grouping brain regions: They clustered brain areas that act similarly, like making teams of players who move together. This captures high‑order cooperation (not just two areas at a time, but groups working together).
- On/off snapshots: For each moment in time, they labeled each group as “on” (active) or “off” (inactive), based on whether the signal was above or below its usual level. Think of it like marking each team as playing or resting each second.
- Building the energy landscape: They used a “maximum entropy model.” In simple terms, it’s a best‑guess model that matches what we observe (how often each team is on, and which teams are on together) without adding unnecessary assumptions. This model assigns an “energy” to every possible on/off pattern:
- Low energy = stable, common patterns (valleys).
- High energy = unstable, rare patterns (hills).
- Tracking brain movement: Over time, they looked at how the brain’s state moved between valleys (stable states) and hills. They measured:
- How often it transitioned between low and high points.
- How big those jumps were (small bumps vs. big leaps).
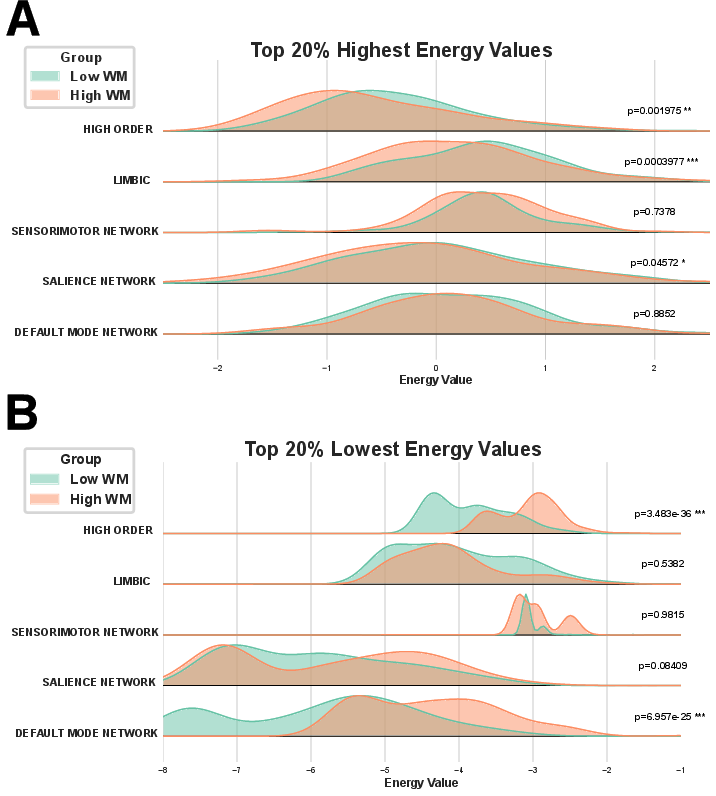
- How extreme the lowest and highest energy states were.
- Testing predictions: They used a machine learning method called a “random forest” (many simple decision trees voting together) to test whether these energy features could predict who would have lower working memory scores six months after surgery.
They studied 20 adults with brain tumors who had fMRI and memory tests before surgery and six months later. Working memory was measured with a standard test called Spatial Span, then grouped into “high” or “low” performance.
What they found and why it matters
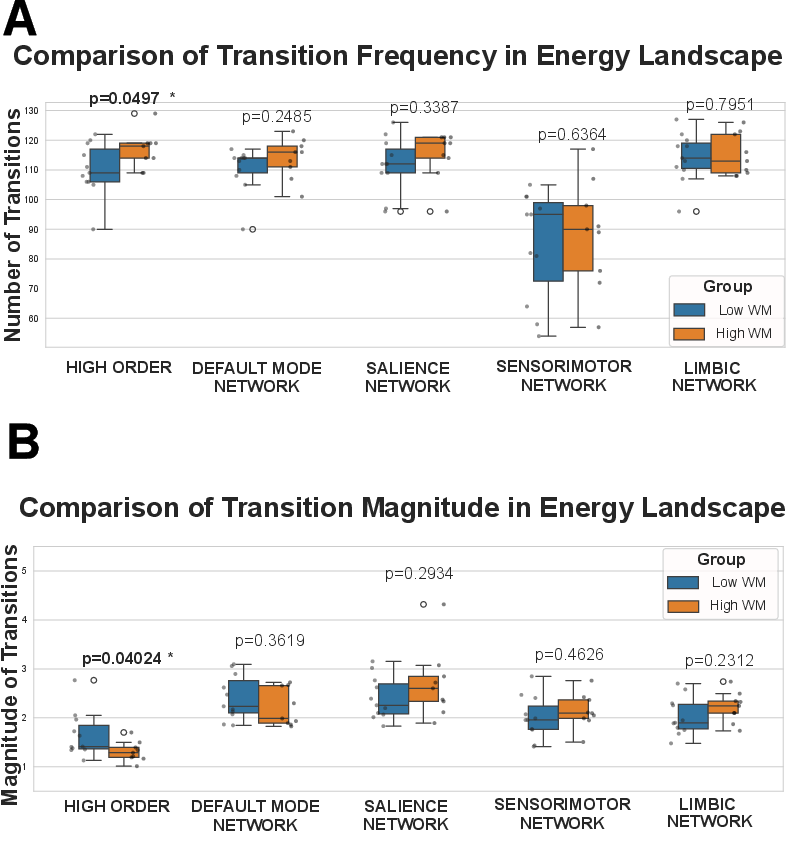
- Different movement styles, different outcomes:
- Patients who later had lower working memory tended to make fewer transitions, but the jumps were bigger and more extreme. Think of a marble stuck in one valley that only occasionally makes a big leap to another valley.
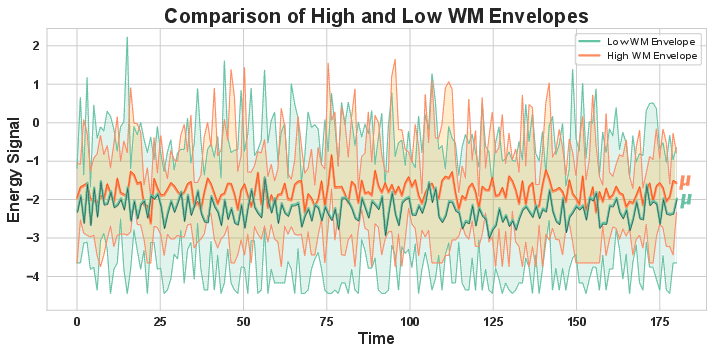
- Patients with better working memory showed more frequent transitions, but the jumps were smaller—more flexible and balanced movement across the landscape.
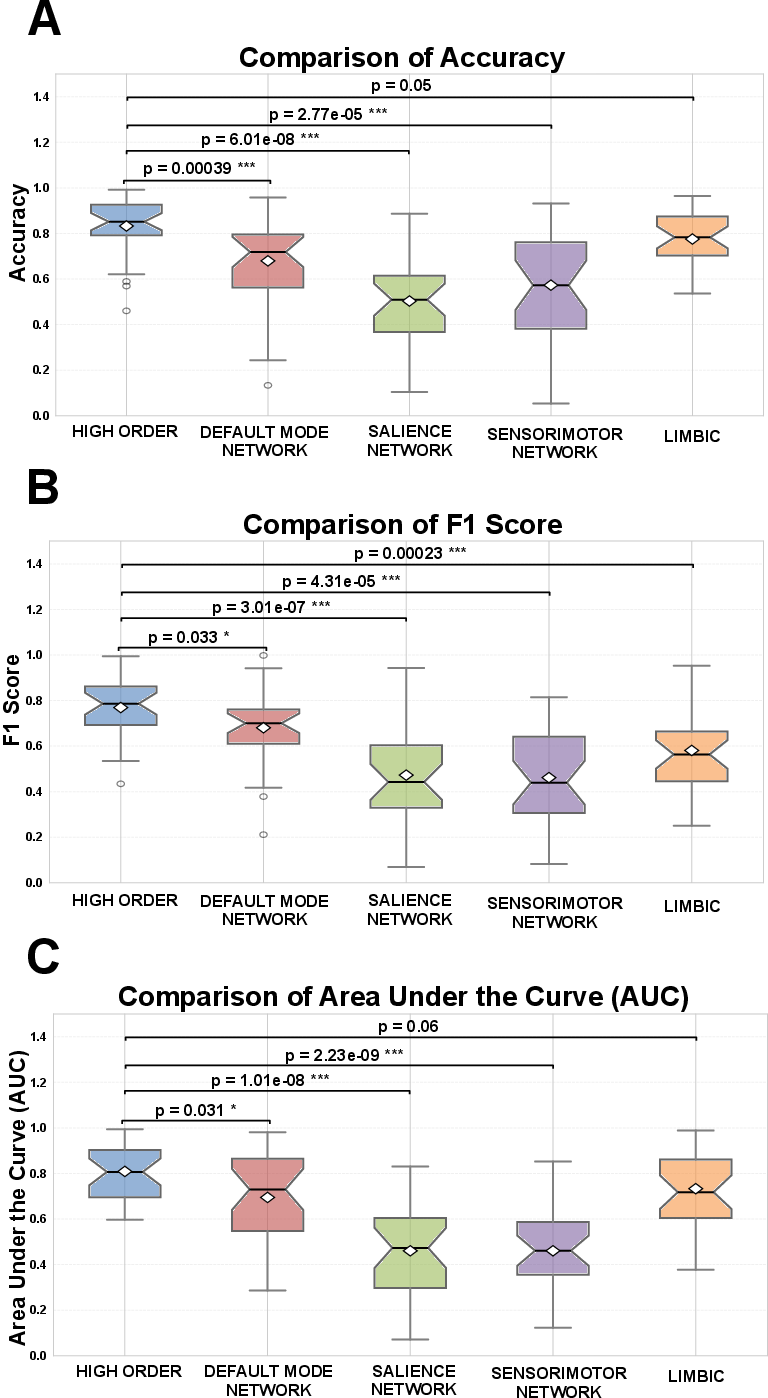
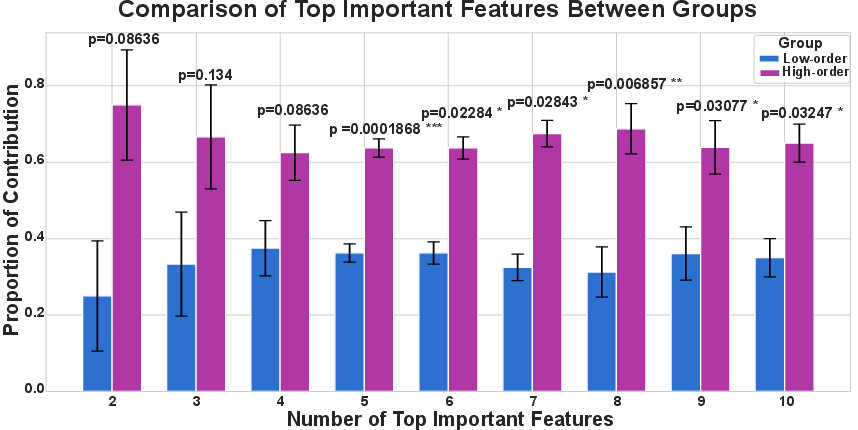
- High‑order features are better: The group‑based (high‑order) energy landscape features did a better job predicting outcomes than traditional, simpler measures that focus on individual networks (like the Default Mode Network or Sensorimotor Network).
- Strong predictive performance: Using just the presurgery energy features, their model reached about:
- 90% accuracy,
- 87.5% F1 score,
- 0.95 AUC (a measure of how well the model separates high vs. low outcome groups).
- These are strong numbers, especially given the small sample size.
Why this matters: If doctors can spot who is at higher risk for memory problems before surgery, they can plan more carefully, offer extra support, and start targeted therapies sooner.
What this could mean in real life
- Better planning: Surgeons and care teams could weigh cognitive risks more precisely when planning tumor removal.
- Personalized care: Patients at higher risk could receive tailored rehabilitation, brain training, or neuromodulation (gentle brain stimulation) to support recovery.
- Earlier support: Knowing the risk in advance helps families and patients prepare and can reduce stress by setting the right expectations.
A simple way to picture it: Imagine the brain’s activity as a marble rolling around a landscape of bowls (valleys) and hills. Healthy, flexible memory tends to move smoothly between nearby bowls. When the brain’s landscape is disrupted (as can happen with tumors), the marble may stay stuck longer and only move with big, effortful jumps. This pattern, seen before surgery, was linked to who struggled more with memory after surgery.
Note: This study used a small group (20 patients), so larger studies are needed to confirm these results. But the early signs are promising and suggest a useful new tool for predicting cognitive outcomes.
Collections
Sign up for free to add this paper to one or more collections.